November 15, 2022
Robert Otto Valdez, PhD, MHSA
Director
Agency for Healthcare Research and Quality
5600 Fishers Lane, 7th Floor
Rockville, MD 20857
RE: Request for Information on Person-Centered Care Planning for Multiple Chronic Conditions
Dear Dr. Valdez:
The National Committee for Quality Assurance (NCQA) thanks AHRQ for the opportunity to provide feedback on person-centered care planning for people at risk for, or living with, multiple chronic conditions.
NCQA is a private, 501(c)(3) not-for-profit, independent organization dedicated to improving health care quality through our Accreditation and measurement programs. We are a national leader in quality oversight and a pioneer in quality measurement. Our mission to improve the quality of health for all Americans, with an intentional focus on health equity, propels our daily work. Leveraging our strengths as a trusted third party, we are committed to helping organizations move toward a more equitable health care system through accountability, transparency and measurement.
We are pleased to provide the following recommendations and feedback for select questions in
this RFI.
What quality of care measurements (e.g., metrics, indicators) exist or are emerging for assessing process, implementation, and outcomes associated with person-centered care planning?
 People with complex health needs, particularly older adults with multiple chronic conditions, serious illness or frailty, often get health care that is fragmented, costly, potentially dangerous and, most important, that may not reflect what matters most to them. Nearly 30% of Medicare beneficiaries have complex health care needs, and more than 14 million people in the U.S. need long-term services and supports. These numbers are growing every year. Existing quality measures do not capture what is most important to individuals, particularly older adults with functional limitations and complex health issues. Appropriate quality of care measures that capture what matters to people are urgently needed to improve and incentivize care for the large and growing group of people with complex health needs.
People with complex health needs, particularly older adults with multiple chronic conditions, serious illness or frailty, often get health care that is fragmented, costly, potentially dangerous and, most important, that may not reflect what matters most to them. Nearly 30% of Medicare beneficiaries have complex health care needs, and more than 14 million people in the U.S. need long-term services and supports. These numbers are growing every year. Existing quality measures do not capture what is most important to individuals, particularly older adults with functional limitations and complex health issues. Appropriate quality of care measures that capture what matters to people are urgently needed to improve and incentivize care for the large and growing group of people with complex health needs.
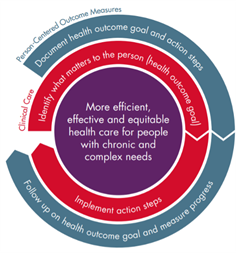
To address this challenge, NCQA, with support from The John A. Hartford Foundation and The SCAN Foundation, developed, implemented and tested Person-Centered Outcome measures. These measures (two process measures and one outcome measure) work in tandem with clinical care to help people living with complex health needs make progress toward a health outcome goal that matters to them. Clinicians across the care continuum—from primary care, to specialty care, to home-and community-based services—can use this measurement approach to elicit what is important to the individual.
After capturing what is important to the individual, the clinician documents a health outcome goal and collaborates with the individual on clinical action steps to achieve it. Person-centered outcome measures standardize the documentation and measurement of progress using Patient-Reported Outcome Measures (PROM) or goal attainment scaling. Within 6 months, the clinician follows up with the individual to assess if they made progress and/or achieved their goal. This approach improves the care planning process and provides valuable data on a range of goals that are important to the individual and their care partners.
| Measure 1: Goal Identification | Measure 2: Goal Follow-Up | Measure 3: Goal Progress/Achievement |
| The percentage of individuals 18 years of age or older with an identified complex care need who identified a health outcome goal, resulting in completion of a patient-reported outcome measure (PROM) or goal attainment scaling and development of an action plan. | The percentage of individuals with an identified complex care need who received documented PROM or goal attainment scaling follow-up care within 180 days of developing an action plan. | The percentage of individuals with an identified complex care need with a documented health outcome goal (using PROM or goal attainment scaling) who made progress or achieved their individualized outcome goal. |
NCQA’s person-centered outcome measures are the result of 10 years of collaboration between NCQA, individuals and their families, clinicians, researchers and 13 health care organizations. The measures were tested in a variety of settings, including Medicaid case management, home-based primary care and general case management, so we could better understand the training and workflow changes needed to provide care that aligns with a person’s health outcome goals.
Findings from our research studies suggest that individuals, care partners and clinicians found the measures to be beneficial and valuable in setting personalized, measurable goals in care visits. Patients felt heard and respected in the design and delivery of care they received. They reported feeling more engaged in their care and having an improved care experience. As a result, they experienced a better relationship with their clinician, which allowed for delivery of personalized care. This approach leads to more efficient, effective and equitable health care for people with chronic and complex needs.
Person-centered outcome measures are gaining interest in clinical areas. This year, NCQA launched a learning collaborative to test the measures’ feasibility in primary care and long-term services and support settings. Due to the large amount of interest in the collaborative, we launched a second collaborative for behavioral health organizations—specifically, 14 Certified Community Behavioral Health Clinics—to complete end-to-end testing of the measures. We are working with experts in the behavioral health field and with participating sites to adapt the measures to fit clinical workflows and the populations of participating behavioral health organizations.
How can equity be ensured in person-centered care planning?
NCQA strives to address inequities in health and promote health equity through performance measurement. To shed light on health care disparities, NCQA stratified 13 of our Healthcare Effectiveness Data Information Set (HEDIS) measures by race and ethnicity. HEDIS is one of health care’s most widely used performance tools, and over 200 million people are enrolled in plans that report HEDIS results. We also released a Social Need Screening and Intervention measure to encourage health plans to assess and address the food, housing and transportation needs of their patient populations.
Our health equity measurement strategy is complementary to our work with Person-Centered Outcome measures, as diversity, equity and inclusion drive our daily work to advance measurement science. The measures focus on encouraging patients to work with their clinician to coordinate their care around what matters most to them. To address equity and care alignment, NCQA is developing and disseminating messages about the measures using information, data and stories that resonate with, and demonstrate value to, a variety of populations and viewpoints. We are adapting training to ensure that this approach can be implemented with diverse populations.
For learning collaborative participants, required data elements for analysis include race, ethnicity, preferred language, social needs, payer and ZIP code. Analysis will reveal differences in measure implementation, follow-up and success across these data elements, and will help us understand if stratification is necessary. While NCQA is using this approach for Person-Centered Outcome measures, the approach also applies to efforts outside measurement that are aimed at advancing person-centered care planning.
Thank you again for the opportunity to comment. We welcome the chance to discuss our experience and findings, and we remain committed to building a better quality, sustainable and responsible American health care system.
If you have any questions, please contact Eric Musser, NCQA Assistant Vice President of Federal Affairs, at (202) 955-3590 or at musser@ncqa.org, or Olivia Umoren, NCQA Federal Affairs Manager, at (202) 827-9450 or at oumoren@ncqa.org.
Sincerely,
Margaret E. O’Kane
President


